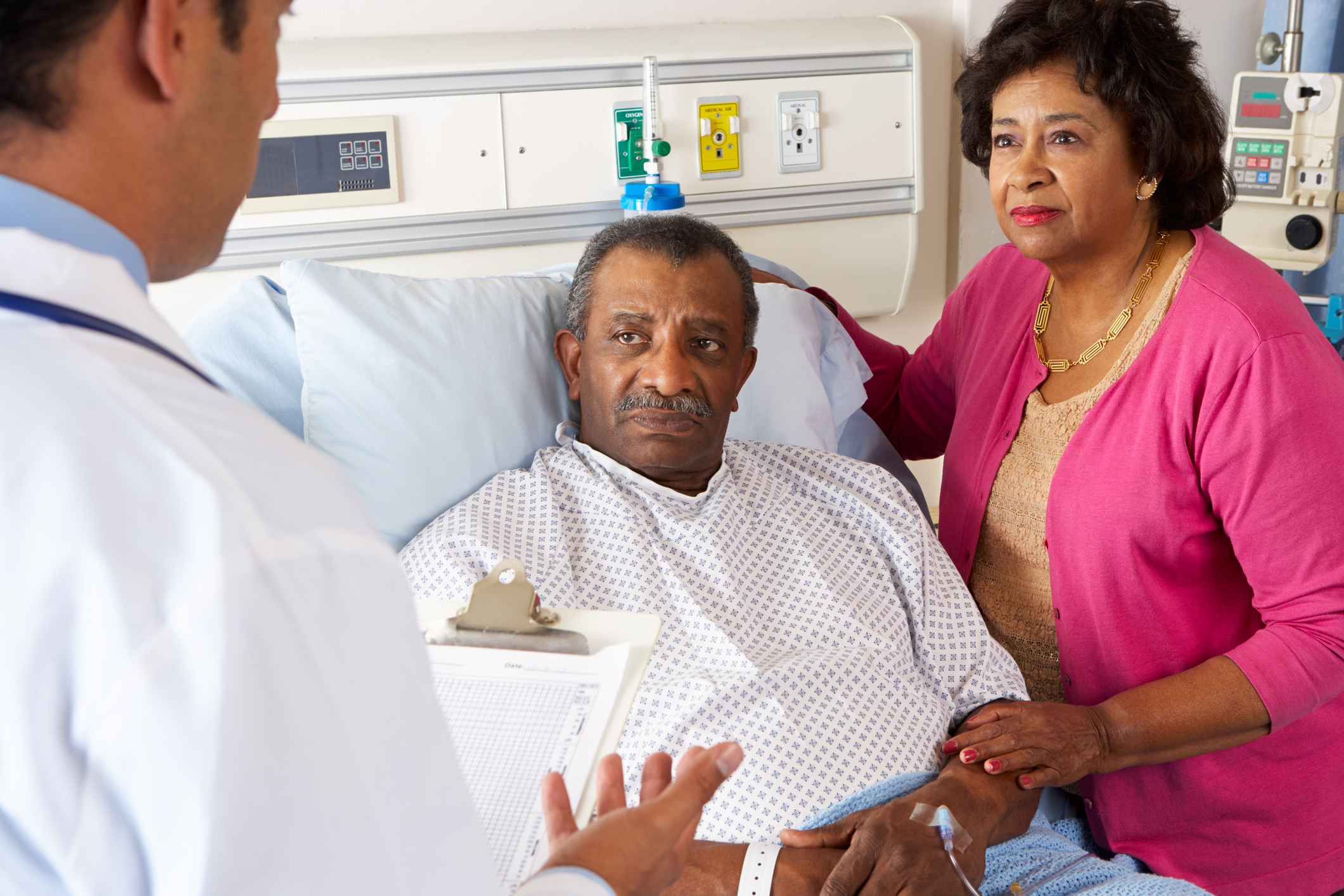
When people feel better, they do better—even when there’s nothing else to be done. Palliative treatment for a serious illness and end-of-life hospice care are ways to manage pain, nausea and weakness. Patients then can spend their days with friends and family or however they’re most at ease.
Diseases of old age cannot be managed forever. When the care team can slow down a progressive condition, they help give patients a longer life. By controlling pain and limiting the side effects of treatment, palliative medicine helps give them a better life. For a complex set of symptoms, doctors may recommend both approaches in combination.
A Holistic Approach to End-of-Life Care
Hospice care brings this compassionate approach to the end stage of life. “Hospice can help with the trajectory of life at the end and a better quality of life,” said gerontologist Karen Wohkittel, Zing Health’s vice president for health services. “It allows people to decide, ‘I don't want to keep going back and forth to the hospital.’ And then they can be in surroundings they’re more familiar with, which is actually much better than being in a hospital.”
As ailments worsen or spread, there can be too many complications to hold back, from labored breathing to confusion and agitation. Hospice puts patients in a comfortable and settling environment, either at home or in a care facility, to treat psychological, social and spiritual as well as medical needs
Hospice care also can comfort family members. They get help dealing with a strange and emotional situation—the inevitable and impending death of a beloved person in their life. There really isn’t an easy way into the subject of human mortality, and many people take the route of avoiding the hard facts and unavoidable outcome. Sadly, avoidance can lead only to regret.
Getting active coaching and support from an end-of-life counselor through hospice organizations can help a family face what’s happening, be present, remove the unease around talking about death and ultimately be more present and create a meaningful experience that will stay with them. They get time to visit with their loved ones, ask about things no one ever talked about during their life and heal some old hurts. Hospice volunteer respite workers can step in when they need a break.
Medicare Advantage and Hospice
Traditional Medicare covers hospice care, even for Medicare Advantage members. They can continue in their Medicare Advantage plan and use the benefit to find hospice facilities, coordinate care and cover palliative medicine or unrelated conditions.
Hospice care can take two forms. Inpatient hospice care takes place in a facility built for that purpose, without the noise and confusion of a hospital and with spaces for family to gather.
With home hospice care, the hospice team can equip a household with the necessary equipment and visit the patient’s home on a schedule. An aide helps with bathing and grooming and can show people in the household how to give better care. They can also provide respite care, short-term relief for hours or days, to give family caregivers a break from around-the clock responsibilities.
“Sometimes people don't elect hospice,” Wohkittel added. “And if they don't, then we work with the family to make sure that there are caregivers in place. If they’re burned out, we can connect them to community resources to give them additional support.”
The typical Medicare patient spends 18 days in hospice. Care can extend for months, though. The care team will rethink treatments that don’t relieve symptoms or improve quality of life. With less potential for drug interactions or side effects, symptoms can improve and patients are able to live with their condition in greater comfort.
Setting the Stage for End-Stage Care
End-of-life care decisions are hard but can’t be avoided. Talking with your care team about the direction of an illness in advance will help them formulate a game plan that gives you the care you expect and deserve.
"People really need to have difficult conversations with their doctor about the progression of the disease and how long can they live with this disease,” Wohkittel said. “It's important to understand what stage you're at and what you can do to improve your life expectancy or improve your condition. When it comes time to really discuss hospice, then the doctor knows your wishes, so they can help direct that conversation.”
There needs to be a discussion in the family too. “They may say, ‘do all the treatment’ but the person may not really want all that,” Wohkittel added. “A pastor or a priest might also help guide members in their decision making.” The Zing Health team will give members help to prepare advance directives, coordinate transitions of care and make sure that doctors, caregivers and ministers are on the same page.
Zing Health’s care team can help members put written advance directives in place to guide their care. The website Five Wishes also can help people think through the range of medical and spiritual questions that might come up in a serious illness.
Talking about end of life can be taboo,” Wohkittel said. “People don't want to talk about dying, they want to talk about living, and people living longer and longer. So, it is a hard conversation and it is scary. But the time to think about it is really before a crisis occurs, when emotions are running very high.”